Despite Technology, Verbal Orders Persist, Read Back is Not Widespread, and Errors Continue
In January 2017, we invited readers of our acute care, community/ambulatory care, long-term care, and nursing newsletters to complete an online survey to learn about the use of verbal orders that are spoken aloud (face-to-face), provided via telephone, or left on voicemail. The survey directed respondents to exclude verbal orders that occurred during order clarifications. We sincerely thank the 1,622 nurses (75%), pharmacists (23%), and other practitioners (2%) who completed the survey! Most respondents practice in a wide variety of hospital settings (87%), including medical/surgical units (31%), intensive care units (21%), inpatient pharmacies (18%), emergency departments (15%), procedural areas (14%), telemetry units (13%), and obstetrical units (7%). The remaining respondents practice in ambulatory clinics (6%), long-term care facilities (2%), community pharmacies (2%), or other facilities (3%).
ISMP conducted this survey to gain insight into the current use of verbal orders in today’s healthcare environment given the increased use of computerized prescriber order entry and electronic prescribing, which have the potential to reduce errors resulting from unclear handwritten and verbal orders. The survey results suggest that verbal orders are still used, and that the critical safeguard of reading back verbal orders for verification is limited. The potential for verbal orders to be misunderstood, misheard, or transcribed incorrectly makes them error prone, particularly given different accents, dialects, and drug name pronunciations by the prescriber and recipient of the order. Add in sound-alike drug names and dosing numerals (e.g., 50 vs. 15), background noise and disruptions, and the failure to seek verification, it is not surprising that errors with verbal orders continue to be reported. Further details about the survey results follow.
Survey Results
Methods used to communicate verbal orders. Most respondents reported receiving verbal orders during the past year via telephone (85%) and spoken face-to-face (74%). While only 4% of nurses and pharmacists reported receiving verbal orders left on voicemail, such occurrences were reported in both hospital pharmacies and patient care units, particularly medical/surgical units, emergency departments, intensive care units, and telemetry units. In community pharmacies, telephone (96%) and voicemail (79%) were the primary modes of communicating verbal orders.
Frequency of verbal orders. For more than a quarter of respondents, at least 1 in every 4 orders is received verbally. Almost 12% of respondents indicated they received more than half of all orders during the past year as verbal orders, and another 14% reported receiving 26% to 50% of all orders as verbal orders. For most of the remaining respondents, verbal orders were received but less frequently—between 6-25% of all orders for 33% of respondents, and between 1-5% of all orders for 40% of respondents. Only 1% of all respondents told us they had not received any verbal orders in the past year.
Read back verbal orders. The Joint Commission (TJC) includes a requirement under the Provision of Care, Treatment, and Services (PC 02.01.03, EP 20) for the receiver of a verbal order to record it and read (not repeat) it back to the prescriber. This helps assure that one has not only heard an order correctly but also transcribed it accurately. Nevertheless, nearly half (45%) of all respondents who reported receiving telephone or spoken orders told us they do this less than 50% of the time. In fact, 16% of respondents said they read back verbal orders only 1-5% of the time, and 9% indicated they never carry out this important verification process. A few respondents commented that their organizations require practitioners receiving verbal orders to repeat back, rather than read back, verbal orders, or that no distinction has been made between repeat back and read back. Others indicated that verbal orders are first written on scrap paper and read back, but then later transcribed or entered into the patient’s actual medical record. 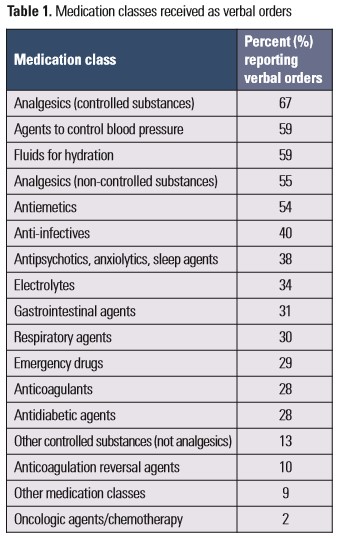
Classes of medications. Respondents also identified medication classes for which they have received verbal orders in the past year (see Table 1), some of which are high-alert medications. Analgesics, agents used to control blood pressure, fluids for hydration, and antiemetics were reported by more than half of the respondents. Despite being highly discouraged by ISMP, 2% of respondents reported receiving verbal orders for oncologic agents/chemotherapy in the past year.
Medication errors. Fourteen percent of respondents were aware of an error that occurred in the past year due to mishearing, misunderstanding, or incorrectly transcribing verbal orders. No trend emerged regarding the type of pharmacy or patient care unit where the errors occurred. Selected examples of the 211 errors reported by respondents are described in Table 2.
Recommendations
Because there are situations in which verbal orders are unavoidable during emergencies or sterile procedures, consider the following recommendations to reduce the risk of an error.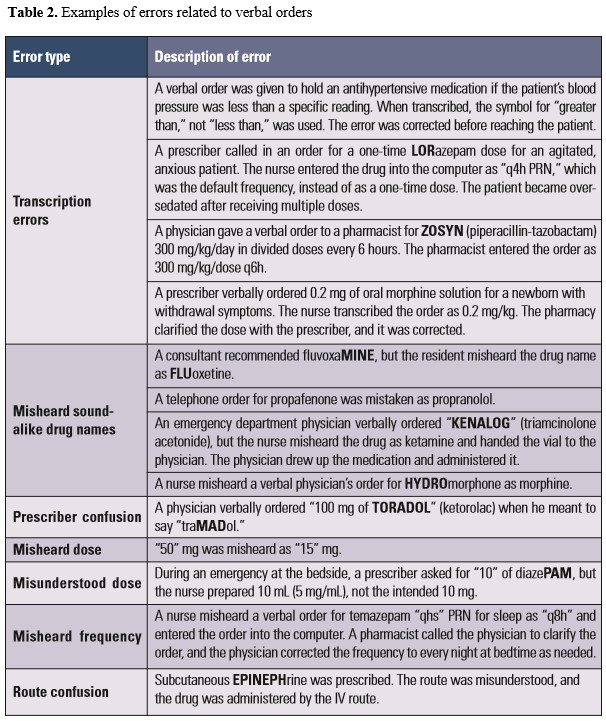
Organizational Policies and Procedures
Prohibit verbal orders for chemotherapy. Do not allow verbal orders for chemotherapy except to hold or discontinue it. These medications are not administered in emergent situations, and the dosing regimens are often complex.
Limit verbal orders. Limit verbal orders to true emergencies or circumstances in which the prescriber is physically unable to electronically transmit, write, or fax orders (e.g., working in a sterile field). For example, except in emergent situations, do not allow verbal orders for entire order sets when admitting or discharging patients or during medication reconciliation when prescribing medications. Do not allow verbal orders for convenience or as a means of circumventing an electronic prescribing system.
Limit to formulary drugs. If verbal orders are necessary, only allow them for items on formulary because the names and dosages of drugs unfamiliar to practitioners are more likely to be misheard.
Define the process. Define the prohibitions and limitations on verbal orders and when they are acceptable; a mechanism to establish the identity and authority of the prescriber; elements of a complete verbal order; and the requirements for clear communication of verbal orders, direct transcription into the medical record or onto a prescription pad, and the readback process for verification.
Prescribers and Receivers
Clarify all communications. Avoid all drug name abbreviations and error-prone dose, route, or frequency abbreviations (e.g., U, IU, SC, QD). Spell out drug names, and for sound-alike drug name pairs, use a phonetic alphabet (e.g., “T” as in “Tango,” “C” as in “Charlie”). Communicate each single dose, not a total daily dose, and pronounce each digit of a number separately (e.g., “sixteen, one six,” to avoid confusion with “sixty”). When appropriate, use leading zeros but not trailing zeros when specifying doses.
Prescribers
Confirm patient and allergies. Before issuing the order, identify the patient using his or her full name and birth date, and confirm the patient’s allergies with the order receiver.
Speak clearly. Enunciate orders clearly and expect (or ask) the receiver to read back the order as transcribed in the patient’s medical record or onto a prescription pad. Provide the indication for the medication to help distinguish between sound-alike medications.
Provide complete orders. Include all elements of a complete verbal order, being clear about the unit of measure for each dose and the frequency of administration.
Repeat order on voicemail. Avoid leaving orders on voicemail in the inpatient setting. If leaving a voicemail in the outpatient setting, repeat the complete order a second time.
Provide weight-based doses. Include the mg per kg dosage along with the patient-specific dose for all weight-based neonatal and pediatric medication orders.
Request patient verification. To verify patient identification, ask the recipient to read back the patient’s name and birth date on the screen or order form/prescription pad that was used to transcribe the verbal order.
Receivers
Transcribe directly into the medical record. Immediately transcribe verbal orders into the patient’s medical record or onto a prescription pad as they are being communicated. Transcription from scrap paper to the medical record introduces another opportunity for error. Based on survey comments, the challenge of directly entering verbal orders into an electronic health record may need to be addressed. For order clarifications by a pharmacist, provide a mechanism for the pharmacist to transcribe the orders directly into the patient’s medical record.
Read back the order. Read the order back to the prescriber for verification. This step is essential and should become habit even if the receiver is confident that he or she has initially heard the order correctly. Although TJC first required this safeguard in its 2003 National Patient Safety Goals, do not assume that this practice is widespread in your facility despite a longstanding policy. Assess how prevalent this practice is in your organization, and take any necessary steps to help practitioners fulfill this safety check. The readback process is perhaps the single most important strategy to reduce errors with verbal orders.
Understand the indication. Ensure that the verbal order makes sense in context of the patient’s condition. This helps to differentiate sound-alike drug names. Record the medication’s indication directly on the order or with the order.
Discourage misuse. Do not accept verbal orders when the prescriber is present and physically able to document the order. Do not accept verbal orders from a “go-between” (e.g., physician office staff) who is not the original prescriber. Do not accept verbal orders for chemotherapy. When telephone communication results in the need to prescribe or change an existing medication, ask the prescriber to transmit the order electronically or by fax, instead of communicating the order by phone.
Do not accept abbreviations. If an abbreviation is given as part of a verbal order, transcribe and read back the meaning of the abbreviation, not the abbreviation. For example, if the prescriber states QID, document and read back four times daily.
